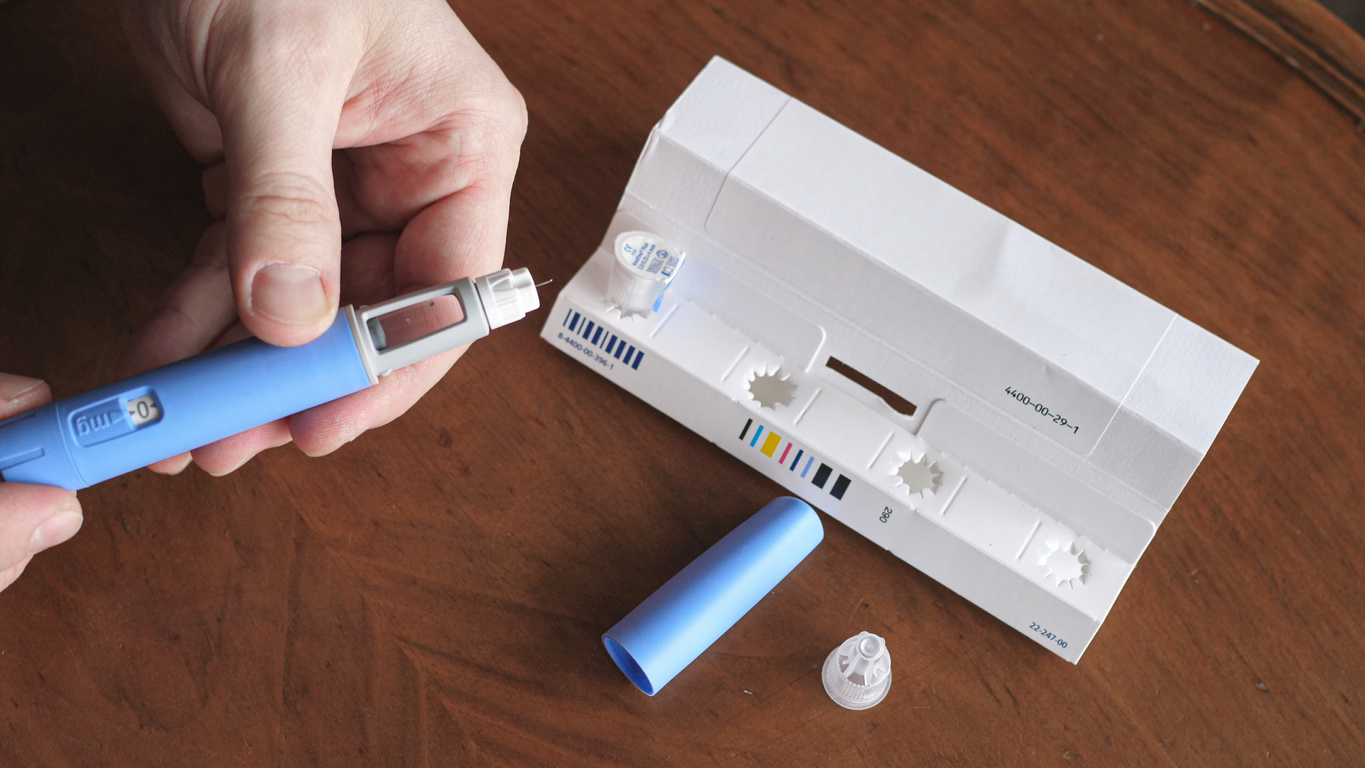
Weight-Loss Solutions of the Future: Next Generation Drugs to Outshine Ozempic’s Results

I have observed how medications like Ozempic, Wegovy, and their predecessors have fundamentally altered the landscape for people with type 2 diabetes and obesity. I am a physician who specializes in obesity and lipid disorders. Meanwhile, there are widespread misconceptions about them, particularly on social media, and many still don’t fully get how they operate. What I do know is that there are additional possibilities on the horizon, some of which may even be more efficient than the medications already available. If you are seeking an ozempic doctor near me, Weight Loss Los Angeles is your first choice.
Mounjaro is one that is now being prescribed, despite the fact that, like Ozempic los angeles, it is currently only FDA-approved to treat type-2 diabetes. Mounjaro, also known as generic tirzepatide, is anticipated to receive FDA approval for weight loss in the summer of 2023. (it seems to be one more large study on safety and efficacy away).
In light of the recent shortages of Wegovy, an FDA-approved drug for the treatment of obesity, Mounjaro is currently prescribed off label, much like Ozempic. Semaglutide, the medication that is in both Wegovy and Ozempic los angeles, is the same; the dosages vary. It has been demonstrated that wegovy can assist people in losing 15% of their body weight. Mounjaro may be able to cause a 21 percent decrease in body weight at specific doses. These outcomes are rapidly becoming close to what is possible with bariatric surgery.
The fact that Mounjaro uses more weight loss techniques than Wegovy could be the reason it is more effective. The medications Ozempic and Wegovy are considered to be glucagon-like peptide-1 (GLP-1) agonists. The intestines naturally create GLP-1, which communicates satiety to the brain. Agonist refers to a drug that attaches to a receptor inside a cell or on its surface and has the same effect as the chemical that typically binds to the receptor. These medications stimulate weight loss because they behave like GLP-1 in the body and can reduce hunger. These medications also encourage the pancreas to create insulin, which can help diabetics lower their blood sugar levels.
On the other hand, Mounjaro is a GLP-1/GIP agonist, which means that in addition to mimicking the glucose-dependent insulinotropic polypeptide (GIP), also called the gastric inhibitory polypeptide, which, like GLP-1, stimulates insulin secretion, and working as GLP-1 in the body. There is disagreement over the exact mechanism at play here, but it’s possible that the presence of GIP boosts GLP-1’s efficiency and has an additional weight reduction effect.
The development of new substances or the combination of new substances that act on multiple receptors in the body connected to appetite, and possibly even metabolic rate, nutrient partitioning (how your body chooses which fuels it stores), and lean muscle mass retention, is the future of obesity medicine. There are a lot of novel chemicals being investigated right now, with the hope that each one will lead to more significant weight loss with fewer adverse effects. There are also plans to develop therapies that don’t require as frequent administration.
CagriSema, which combines cagrilintide with semaglutide, appears to have a lot of potential. Cagrilintide mimics amylin, a pancreatic hormone that similarly affects satiety.
Another is the GLP-1/GIP/glucagon agonist retatutride. Similar to tirzepatide, but going a step further by including glucagon agonism, is this substance. Together with suppressing hunger, it’s probable that the additional glucagon agonism aids in energy expenditure, enabling individuals to burn more calories.
In addition to the new substances under investigation, existing trials are examining the tolerability of greater doses of the available GLP-1 agonists. And while the majority of these substances are initially examined and authorized for type-2 diabetes before being explicitly studied and approved for obesity, that order may be shifting. It appears that a substance by the name of AMG-133, a GLP-1 agonist with an antibody that, unlike tirzepatide, suppresses GIP rather than raising it, is being researched first for obesity.
Although it may seem so, these medications weren’t created overnight. Wegovy, Mounjaro, and Ozempic are the fruits of years of study and development. Every few years, a new molecule has entered the market since the first GLP-1 agonist was licensed in 2005. Exenatide (Byetta) came first, followed by liraglutide (Saxenda and Victoza), dulaglutide (Trulicity), semaglutide (Ozempic and Wegovy), and tirzepatide (Mounjaro).
It’s imperative to clarify the situation before the release of the next generation of medications: this isn’t merely an out-of-control weight-loss trend supported by the pharmaceutical industry. Let me dispel a few of the many fallacies that surround these not-new but recently popular medications.
Misconception 1: Drugs like Ozempic and Mounjaro shouldn’t just be used for weight loss.
Obesity is a long-lasting illness. The body fights back when people try to reduce weight, and excess weight is linked to an elevated risk for a number of health conditions, including type-2 diabetes, cardiovascular events, Covid-19 difficulties, and more. As a result, it has been classed as such since the 1990s.
Nonetheless, our society has long stigmatized those who are obese. They have been informed that their weight is merely a result of their inability to engage in healthy eating and activity. The stigma associated with obesity, which permeates everything from TV entertainment to healthcare, is largely to blame for this.
“Even when using these medications, people still need to maintain a healthy lifestyle and work hard to lose weight. Nonetheless, they can succeed without beginning at a disadvantage.
People with larger bodies suffer from weight stigma in a variety of ways. According to research, those who are considered obese are more likely to face prejudice at work and be fired from healthcare settings. But, there is also stigma associated with receiving medical treatment for obesity, whether it be bariatric surgery or, more recently, the use of an FDA-approved weight loss medicine, which damages those with larger bodies. When nothing could be further from the truth, it is viewed as a “crutch” or “the easy way out”. People with obesity should not be made to feel guilty for taking medications to address their weight, just as you wouldn’t tell someone with type 2 diabetes to feel bad for injecting insulin.
The idea that people shouldn’t use GLP-1 agonists for weight loss alone is a significant myth. It’s true that the majority of GLP-1 agonists on the market are approved as type-2 diabetes medications and not all of them have been approved for obesity yet. We know that Ozempic (the same substance) is safe and effective for weight loss because semaglutide (in its Wegovy form) was FDA-approved especially for the treatment of obesity in 2021.
People can consult their doctor to see whether an off-label prescription is appropriate for them if they are experiencing Wegovy shortages. Those who are obese have the same right to access to medication that can help them manage their condition as everyone else. Obesity should be treated with the same seriousness as any other sickness.
Misconception 2: You can use these medications to reduce your weight and then stop.
Another common misconception regarding these medications is that they can be used as a “quick cure” to help you lose weight and then you can stop using them. In actuality, they only function if you constantly take them, much like a blood pressure medication or other medications for a chronic illness. Since they are supposed to be used continuously, stopping and starting these medications can have an uncontrollable yo-yo effect on appetite and weight. Some people might be able to wean themselves off of these medications, but many will need to continue taking them at least at a low level.
These drugs enable people to lead the lifestyles they already know are necessary to reduce weight by affecting appetite regulation, one of the keys to long-term weight loss. The majority of people are aware that if they’re trying to lose weight, eating an apple instead of chips is usually a smart choice. But given that they know how to do it, why can’t they? It’s because persons with a genetic propensity for obesity are especially susceptible to the brain’s ability to encourage them to eat larger portions and high-calorie foods. With these foods, some people are able to use moderation. Some folks are able to refrain. Despite their best attempts, many people cannot.
Those who struggle with obesity, even receiving the best coaching and assistance available, report feeling what it must be like to not struggle with hunger and weight after taking these medications. “Normal,” they claim to feel. People still need to adopt a healthy lifestyle and put in a lot of effort to reduce weight. They can succeed without beginning at a disadvantage, though.
“Diet and exercise only help a small percentage of obese individuals who wish to reduce weight, it is a reality. There is now another choice thanks to these new tools.
If we let it, obesity medication has the potential to significantly enhance the lives of people with obesity-related health issues. However, just 30% of insurance companies will pay for these treatments, which is another way that the stigma associated with obesity and the false belief that it is solely a lifestyle problem harms people.
Misconception 3: Whether you’re attempting to reduce 15 pounds or 100 pounds, these drugs are fantastic.
These medications shouldn’t be sought out by those who haven’t been diagnosed with type 2 diabetes or obesity. That not only makes it more difficult for those who truly need these medications to get them but also poses hazards. If someone who wants to drop a few pounds takes them, they can become underweight and lose bone and muscle mass instead of extra fat. Although the medications are generally safe, there is a chance of unpleasant side effects, particularly nausea.
A licensed doctor must supervise the use of these drugs. In particular, if they are prescribing a medicine from a compounding pharmacy, I wouldn’t trust a doctor who is assisting you in obtaining something you don’t actually need (one that not only distributes drugs but makes them, which introduces risk of contamination).
Diet and exercise are notoriously difficult to maintain, therefore they only help a small percentage of obese people who wish to lose weight. These new tools give patients another option—one that’s reasonably safe, non-invasive, and successful—to help them lose weight and keep it off without having to fight constantly.
Weight Loss Los Angeles | Ozempic Doctor Near Me
Everyone ought to have complete autonomy over their own body at the end of the day. Nobody should ever be pressured to lose weight or treated differently for their size if they are obese but otherwise healthy and content. Yet, folks who are struggling and are in need of change shouldn’t be made to feel ashamed or face obstacles to getting access to resources that can be helpful.
If you are seeking an ozempic doctor near me, contact our team at https://www.weightloss-losangeles.com/.